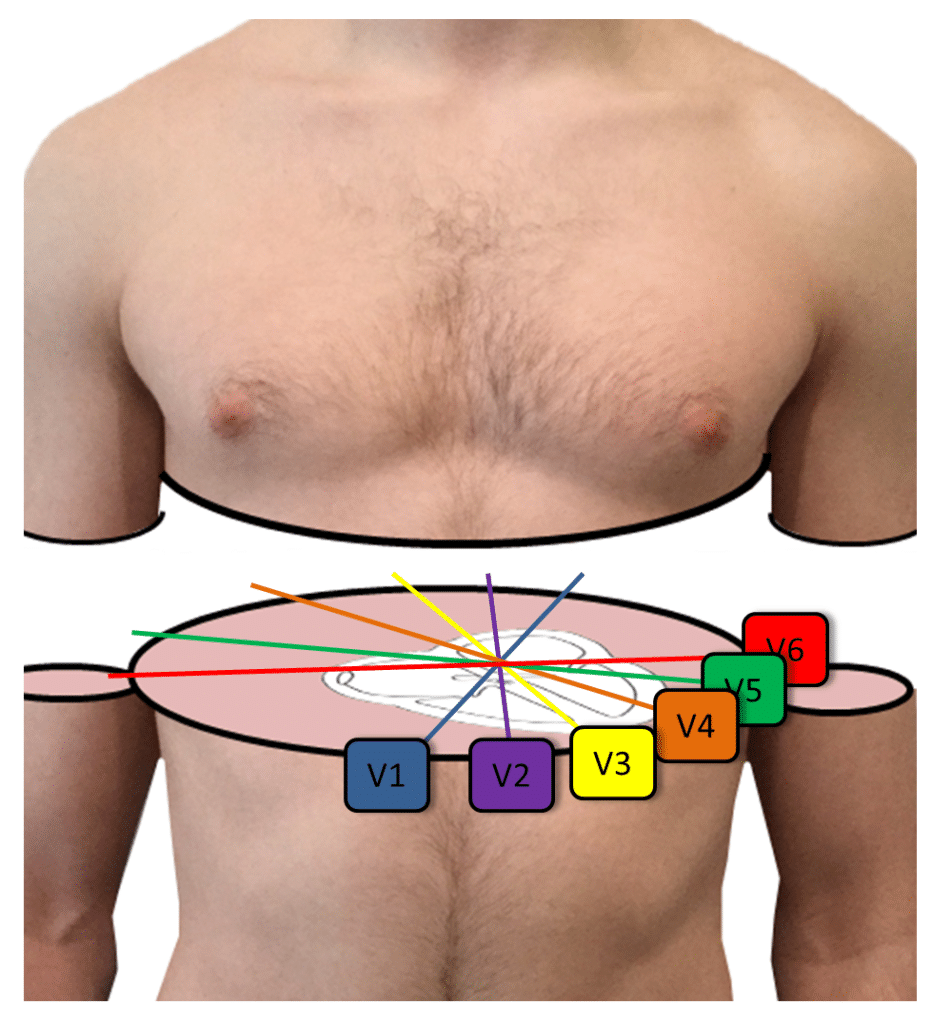
In all patients, the accuracy (percentage of patients with an exact prediction of AP-localization) of the EASY-WPW algorithm was superior compared to the PAMBRUN (93% vs. Direct comparison of the accuracy of AP-algorithms. Pericardial effusion (PE) was ruled out immediately after ablation and the next day.ĭirect comparison of AP-algorithms. Persistent ablation success was confirmed after a waiting period of 30 min by adenosine administration. 
During left-sided AP-ablation intravenous heparin was administered to maintain an activated clotting time (ACT) of 300 s throughout the procedure. 
Vascular access (femoral vein or artery), additional material (long sheath for catheter stability), and energy source (standard radiofrequency, irrigated radiofrequency, or cryothermy) varied with ablation site. The ablation catheter choice depended on the AP-localization and physician preference. 
During EPS, pathway location and characteristics were determined. The third diagnostic catheter was positioned in the apex of the right ventricle (RV). One diagnostic catheter was placed in the coronary sinus (CS), while the other diagnostic catheter was positioned at the His bundle. Antiarrhythmic drugs (AADs) were discontinued at least three half-lives before ablation.įor EPS, three diagnostic catheters were percutaneously inserted through the femoral vein. We aimed to retrospectively develop, prospectively test, and externally validate a novel, simple 12-lead ECG-based algorithm considering the patients’ heart axis allowing for an accurate and reliable pre-interventional AP-site localization in adults and children.Īll procedures were performed under conscious sedation using propofol and analgesia with fentanyl as required. 11–14 As WPW is the most common cause of tachycardia in children, 2 a more sensitive and reliably applicable AP-algorithm in pediatric patients is strongly required. 4–10 However, they have shown to be complex, time-consuming, and often unprecise because of a variable anatomical heart axis, especially in children. Thus, several algorithms for AP-localization primarily including the polarity of delta waves, the QRS complex, or both, have been developed. 3 For optimized patient education, ablation planning and performance pre-interventional determination of AP-localization is desirable. In case of recurrent or severe symptoms, an electrophysiological study (EPS) followed by an AP-ablation is recommended. Typical 12-lead electrocardiogram (ECG) characteristics of WPW include a short PR-interval, a delta wave, and a wide QRS complex. In some patients, WPW is an incidental finding as they are completely asymptomatic, whereas others develop palpitations, atrial fibrillation, syncope, or life-threatening ventricular fibrillation. Wolf-Parkinson-White syndrome (WPW) is characterized by the presence of an accessory pathway (AP) between the atrium and the ventricle. The accuracy of EASY-WPW was superior compared to the Pambrun (93% vs. Our algorithm was particularly useful in correctly localizing antero-septal/-lateral (sensitivity and specificity 100%) and posteroseptal (sensitivity 98%, specificity 92%) AP in proximity to the tricuspid valve. Prediction of AP-localization was correct in 197 patients (93%) (sensitivity 92%, specificity 99%, PPV 96%, and NPV 99%). All patients (32 ± 19 years old, 47% female) underwent successful pathway ablation. The algorithm was developed retrospectively and validated prospectively by comparing its efficacy to two established ones ( Pambrun and Arruda). Our multicentre study included 211 patients undergoing ablation of a single manifest AP due to WPW between 20.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
